
Experiencing back pain? You’re not alone: about 84% of adults face lower back pain at some point in their lives. But it’s important to get to the root and figure out what’s causing your lower back pain, rather relying on painkillers that only relieve the ache for a little while.
Why Lower Back Pain is Common
The flexibility of the lower back increases its susceptibility to injuries. In addition, the nerves that run throughout the spine also go through the rest of your body. Consequently, a problem in your lower back can lead to leg pain, hip problems and more.
Types of Lower Back Pain
According to a 2014 study, there are three main types of lower back pain: acute pain, subacute pain, and chronic pain. Acute lower back pain is pain that lasts for up to four weeks. Subacute lower back pain lasts between four and 22 weeks, and may develop into chronic back pain, which persists for 12 weeks or longer.
Rarely, back pain can be a symptom of serious medical illnesses. Therefore, it’s a good idea to consider the potential causes of your lower back pain.
What Causes Lower Back Pain?

Nonspecific Back Pain
Up to 85% of lower back pain cases are nonspecific, meaning that the person has back pain in the absence of a particular underlying condition. Many such cases are related to musculoskeletal pain and usually improve within a few weeks.
Less than 1% of lower back pain has serious causes, such as cancer or an infection. Less than 10% of lower back pain is associated with less serious causes such as vertebral compression fracture, radiculopathy, or spinal stenosis.
Spinal Cord Compression
According to a 2014 study, pain is usually the first symptom of cord compression, but most people with lower back pain experience motor problems, often involving weakness. Depending on what part of the spine is affected, the person may experience bowel and/or bladder dysfunction.
A 2014 systematic review found that spinal cord compression was caused by an intervertebral disc in 22.7% of cases, ankylosing spondylitis in 15.9%, lumbar puncture in 15.9%, a trauma in 7.6%, a malignant tumor in 7.2%, a benign tumor in 5.7%, and infection in 5.3%.
Lumbar Spinal Stenosis
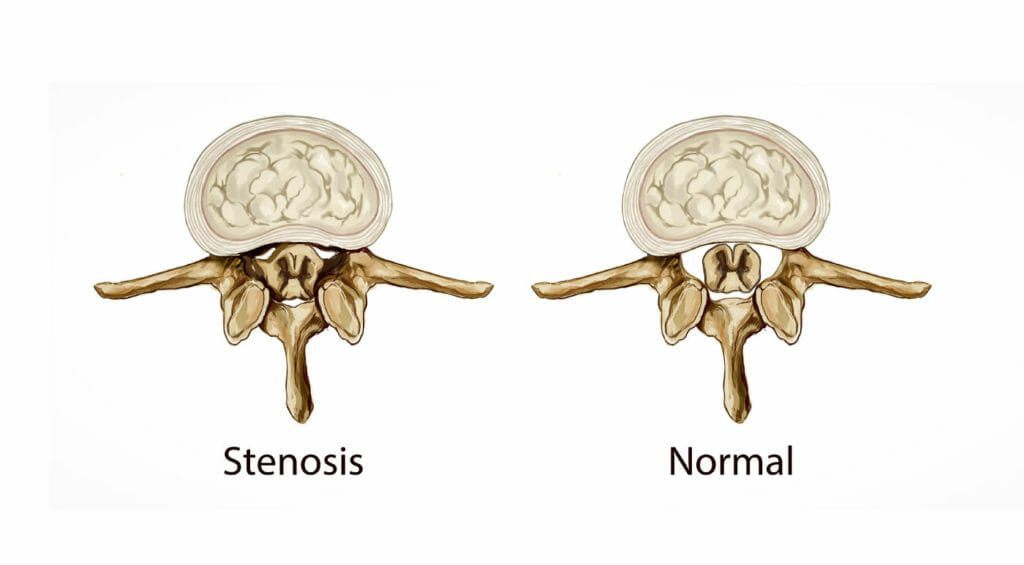
Your lumbar spine (the lower back) consists of five vertebrae, which sit between the ribs and the pelvis. Lumbar spinal stenosis involves the compression of the nerves that serve the lower back, causing pain through the lower back and the legs.
Muscle or Ligament Strain
A strain is an injury to the muscle or tendons that connect the muscles to the spine. Strains occur due to improper lifting or stretching, or by lifting something very heavy that tears the muscle.
Bulging or Ruptured Intervertebral Discs
There are a total of 23 discs in the human spine that cushion the bones, absorb shock between the vertebrae, and prevent trauma during activity by keeping the vertebrae separated. They also protect the nerves that run down the middle of the spine.
A study found that patients with both degenerated discs and related ruptures had a 86.7% chance of lower back pain incidents, much higher than the rest of the patient population.
Arthritis
Arthritis is a degenerative disease that involves the inflammation of one or more joints. Inflammation in the spine results in back pain. A study found that lower back pain and rheumatoid arthritis coexisted in 64.5% of the patients.
Osteoporosis
Osteoporosis involves low bone mass and damage to the bone tissue, which increases the risk of vertebral fractures. A recent study found that most of the osteoporotic pain happens at rest compared to during activities. Treatment of osteoporosis can improve pain outcomes, but it can cause lower back pain.
Can the Way You Sleep Cause Lower Back Pain?

Bed and Mattress
A mattress that’s too soft leaves your pressure points unsupported, creating spinal curvature. A mattress that’s too firm pushes on those pressure points. Both situations result in back pain. According to one study, a medium-firm mattress improved pain and was therapeutically effective for chronic nonspecific lower back pain.
We’ve done the research and collected a list of the 10 best mattresses for back pain.
Sleeping Position
Your sleeping position affects many aspects of your sleep and rest. Proper rest is impossible without the right position that promotes the body’s ability to heal. The wrong sleeping position can put extra stress on your lower back, making the situation worse. For example, sleeping on your stomach can cause back pain.
How to Sleep to Alleviate Lower Back Pain
Support Your Spine
If you sleep with your head propped up too high on the pillow, you can compromise your spine. If you have a history of back pain, you can use a pillow to stabilize your spine and relieve the pressure from your hips and lower back.
It’s also important to ensure you have the right mattress and pillow to get the support and comfort your body needs for optimal rest.
Avoid Sleeping on Your Stomach
Sleeping on your stomach causes excessive curvature of your spine, leading to nerve irritation that can result in lower back pain and discomfort. Even if you have been sleeping on your stomach for a long time, it’s possible with a little practice. You will retrain your muscles to like other safer positions, and in the long run, you’ll sleep better. If you have difficulty making the switch, try using a body pillow.
Consider Other Factors That Affect Your Sleep
When clients consult me for a sleep problem, I facilitate an integrative holistic assessment of all their individual circumstances that could negatively affect their sleep quality. I assess five aspects of sleep, lifestyle habits, nutrition and potential nutritional deficiencies, hormones, thyroid function, and gut health. Addressing other aspects of your lifestyle and health will ensure you get high-quality sleep, which can drastically lower your pain levels.
Risk Factors for Lower Back Pain
Age
As we grow older, our bones become fragile, our muscles lose elasticity, and our discs lose cushioning fluid. A survey found that post office workers aged 70 to 75 who had lower back pain had also regularly lifted heavy weights as part of their work for more than 20 years.
Fitness Level and Weight
Back pain is more common among people who are not physically fit, because weak back and abdominal muscles may not properly support the spine. A 2016 study also concluded that obesity resulted in high levels of lower back pain.
Pregnancy
Lower back pain is common during pregnancy as a result of pelvic changes and alterations in weight loading. Back symptoms almost always resolve postpartum.
Improper Lifting

Heavy or improper lifting can overstretch or twist the spine. A prospective study of retired adults aged 58 to 67 showed that previous occupational mechanical exposure to bending, twisting, or driving for at least 10 years increased the odds of having persistent lower back pain.
Smoking
A cross-sectional study concluded that frequent exposure to smoking results in a higher prevalence of lower back pain.
Genetics
Some causes of back pain, such as ankylosing spondylitis, a form of arthritis that involves a fusion of the spinal joints leading to some immobility of the spine, can have a genetic association
Occupational Risk Factors
Having a job that requires heavy lifting, pushing, or pulling, particularly when it involves twisting or vibrating the spine, can lead to injury and back pain. An inactive job or a desk job may also lead to or contribute to pain, especially if you have poor posture or you sit all day in a chair with inadequate back support.
What Kind of Stress Causes Lower Back Pain?
Stress, including both physiological and mental stress, can affect the body in numerous ways, such as causing muscle tension. Physiological stress can arise from direct trauma to the body, such as being in a car accident. Physiological stress can manifest from repeated activity without rest or proper stretching. This happened to me when was training frequently with inadequate stretching between training sessions. As I improved my stretching routine, my lower back pain subsided and did not become chronic.
Importantly, psychological stress can also lead to a buildup of tension, which can cause or worsen lower back pain.
In theory, the body reacts to stress using the same mechanism, regardless of the source of the stress. The body reacts to stress by increasing the stress hormone cortisol, which has an inverse relationship with melatonin, the hormone that helps initiate sleep. Numerous studies have found that uncontrolled stress leads to poor sleep quality.
Sleep Deprivation and Pain
Pain prevents relaxation and stimulates the nervous system, both of which make it harder to sleep. Similarly, not sleeping well means losing out on the healing and body rejuvenation reliably proven to reduce pain.
During sleep, the body repairs damaged tissues, reduces inflammation, and builds muscles. Sleeplessness increases the intensity and frequency of pain, so resolving insomnia is an important goal to help relieve lower back pain.
Can Lifestyle Changes Help You Reduce Lower Back Pain?
Safe exercise, quitting smoking, maintaining proper body mechanics, and improving your sleep can all help you reduce your lower back pain. While many factors affect your sleep, improving your sleeping environment, choosing the right mattress, and choosing a suitable sleeping position are important steps you can take to upgrade your sleep quality and help alleviate your lower back pain.
According to a recent study, exercise is safe for patients with back pain, and in fact, exercise is a proven therapeutic tool for improving flexibility and strength. Depending on the specific type of and reason for your lower back pain, you may need specific types of exercises. That brings us to…
When to See a Doctor for Lower Back Pain
According to clinical review studies, most cases of lower back pain are nonspecific back pain, which tends to last for less than four weeks (acute and subacute pain). This type of lower back pain will typically improve over a few weeks with self-care and lifestyle changes.
If your lower back pain lasts for more than 12 weeks (chronic pain), you should definitely see a doctor to investigate underlying causes.
The clinical evaluation of lower back pain includes evaluating your medical history and assessing physical symptoms. A study found that most patients with acute lower back pain do not require laboratory testing or medical imaging, such as MRI or X-rays. In fact, clinical studies actually recommend that doctors limit the use of medical imaging unless there are specific symptoms that make it necessary, due to the potential for false negatives that could lead to an incorrect diagnosis and treatment.
Additional Back Pain Resources:
The Best Mattresses for Back Pain
How to Sleep With Lower Back Pain
Top 10 Best Mattresses for Seniors with Back Pain