
Time for a pop-quiz. Are you suffering from disrupted sleep? Do you snore loudly? Has your partner told you that you choke and gasp for air during the night? Do you feel like, no matter how much you sleep, you still wake up tired? Are you even becoming more forgetful than you used to be?
If you answered “yes” to most or all of these questions, you could be suffering from sleep apnea. The term might be foreign to some of you, which is why we decided to give you the inside scoop on sleep apnea, including symptoms, causes, and treatments.
What Is Sleep Apnea?
Sleep apnea is a sleep disorder that interrupts breathing during sleep. Sleep apnea happens when the brain fails to properly signal warning lights to your breathing muscles, or when your upper airway narrows, thus blocking air’s entry into the lungs. Needless to say, it’s not exactly the most comfortable of situations to be in. But you might be asking yourself, what causes this mass mis-communication to occur inside your body?
Types of Sleep Apnea
Now that we’ve clued you in on what sleep apnea is, let’s talk about the different types of sleep apnea someone might be dealing with–and how to spot the difference.
Obstructive Sleep Apnea Syndrome

Obstructive sleep apnea syndrome (OSAS) is a complete or partial airway obstruction. The soft tissue in the throat collapses leaving no space for air to flow into the lungs, leading to a complete stop in breathing. OSAS is the most common, and most dangerous, form of sleep apnea.
The sleeper may stop breathing 8 to 100 times in a single night, for a minute or longer each time. These breath stoppages don’t always wake up the sleeper, so they may be completely unaware of the issue. Instead, they wake up with headaches and experience daytime sleepiness, increasing their risk of drowsy driving–not to mention other, long-term side effects like depression.
Central Sleep Apnea
Central Sleep Apnea occurs when the brain fails to send proper signals to the muscles that control your breathing rhythm. A 2013 study found that central sleep apnea is more common in people with congestive heart failure and who use opioids, as well as those who live at altitudes above 6,500 feet.
Complex Sleep Apnea Syndrome
Complex sleep apnea syndrome happens when a person has both obstructive sleep apnea and central sleep apnea. This combination requires urgent treatment, as you can very well imagine.
What Causes Sleep Apnea?
Causes of sleep apnea include genetic syndromes, obesity, smoking, large tonsils, endocrine conditions (such as irregular heartbeats), neuromuscular diseases, and/or premature birth. While some of these factors are out of your control, others are more health-choice related. Let’s do a deeper dive into these causes and how they lead to sleep apnea.
Genetic Syndromes
Some studies have explored the role of genetic predisposition in determining people’s sleep apnea risk and outcomes. Even though we need more research in this area, understanding your family history can help with early diagnosis and treatment.
Obesity

Excess body weight and a sedentary lifestyle result in the slow circulation of blood. Researchers estimate that nearly 25% of adults have sleep apnea, and around 45% of sleep apnea sufferers are obese. Fat deposition in the upper airway results in a narrower lumen, obstructing breathing as stated in this 2019 study, and increases the likelihood of obstructive sleep apnea. In another study a 10% increase in weight was associated with a six-fold increase in risk of obstructive sleep apnea.
Smoking
Studies have not proven a causal relationship between sleep apnea and smoking. However, smoking can worsen your risk of sleep apnea as well as the outcomes. Smoking can obstruct the upper airway through related fluid retention and upper airway inflammation.
Large Tonsils
Large tonsils reduce, and can even block, the airway passage between your mouth, throat and lungs, making it hard for the air to pass through. Since the tonsil is made of lymphatic tissue, it is likely to increase even more in response to infection, making a severe case of OSAS.
Endocrine Disorders
Endocrine disorders have been implicated in Obstructive Sleep Apnea because they share similar clinical features. These disorders can include Hypothyroidism and Goiter.
Hypothyroidism
Hypothyroidism, one of the most common endocrine disorders, is characterized by snoring, excessive daytime sleepiness, fatigue, apathy, frequent headaches, and memory impairments and is often associated with obesity or depression; as pointed out in this recent review , these are also seen in individuals with Obstructive Sleep Apnea.
Goiter
Goiter is an abnormal enlargement of your thyroid gland. Among other symptoms, this can cause upper airway compression leading to difficult breathing, which is also an indicator for Obstructive Sleep Apnea. In cases of shared symptoms, research recommends considering sleep apnea treatment all while addressing the underlying endocrine problem.
Neuromuscular Conditions
Neuromuscular conditions involve respiratory and upper airway muscle weakness, leading to airway obstruction and obstructive sleep apnea. Daytime sleepiness and tiredness may be assumed to originate from lack of muscular strength and overall impact from neuromuscular disorder, therefore contributing to undiagnosed Sleep Apnea
Premature Birth
Babies born prematurely are at increased risk for developing sleep apnea. A 2012 analysis of a nationwide dataset from Taiwan found that pregnant women with obstructive sleep Apnea have almost a 2.5-fold higher rate of preterm birth relative to mothers without Obstructive Sleep Apnea.
Similarly, a recent study summarized a growing body of evidence that sleep disorders, including sleep apnea, increases the chance for premature birth and even death. There is strong evidence showing that better sleep during pregnancy leads to the best health outcomes for both the mother and the baby.
Risk Factors Associated With Sleep Apnea

Males in general are also more prone to sleep apnea than females, as are those of older age, individuals who already deal with nasal congestion and narrow airways, smokers, avid alcohol drinkers, and, of course, those with a family history of sleep apnea.
Men and Sleep Apnea
Men experience Obstructive Sleep Apnea two to three times more often than females, although this study found that the risk appears to be similar once women are postmenopausal. In a 2001 study, central sleep apnea was more prevalent in males than in women. In the study, central apneas were detected in 7.8% of men and only 0.3% of women.
Older Age
According to a recent study, Central Sleep Apnea is more prevalent in people over 65 years of age. The study also pointed out that the risk could be associated with common factors that affect breathing during sleep in older adults. These factors can include heart failure, atrial fibrillation and cerebrovascular diseases. Overall, the risk for sleep apnea increases with age in combination with common risk factors.
Nasal Congestion
According to this study, nasal congestion counts for an approximately two-fold increase in the prevalence of OSAS compared with controls, regardless of the cause. However, OSAS may or may not improve with correction of nasal congestion.
Narrow Airway
Narrowing of the airway is the main cause of obstruction and the inability to breath during sleep. Common obesity, or those with thicker necks, are known to be a main cause of narrow airways.
In one study, narrow airways can be due to health problems such as tonsillar hypertrophy, a high arched or narrow palate, nasal septal deviation, and nasal polyps.
Alcohol, Sedatives, and Tranquilizers
According to this study, alcohol consumption increases the frequency and duration of Obstructive Sleep Apnea episodes. Sedatives and tranquilizer medication also relax throat muscles, increasing chances for airway obstruction or worsening Obstructive Sleep Apnea.
Family History and Genetics
According to a 2014 study, even just the shape of someone’s airways are hereditary and can increase the risk for Obstructive Sleep Apnea beyond lifestyle-related risk factors. This is why sleep apnea in children often involves correcting any anatomical abnormalities in order to set a better foundation for a healthy life ahead.
Symptoms of Sleep Apnea

Sleep apnea, as we’ve stated, is commonly characterized by snoring, irregular or even temporarily stopped breathing occurring several times during sleep. But other daytime drowsiness, decreased interest in sex, forgetefulness, mood changes, morning headcahe, and nighttime urination are also behavioral changes caused by sleep apnea that might mask themselves as just you having a rough week. But, in reality, your health could be in serious jeopardy.
Decreased Interest In Sex
There is strong research evidence that erectile dysfunction and sexual dysfunction are more common in men with sleep apnea. In this study, 69% of male participants diagnosed with Obstructive Sleep Apnea also had Erectile Dysfunction. But what is the science rationale behind this connection?
Sleep deprivation leads to a decline in testosterone levels. Alternatively, low testosterone levels can lead to sleep disturbances, as shown in this 2014 study. Testosterone and oxygen are (not surprisingly) both important for healthy erections. But sleep apnea cuts off oxygenation and further disrupts sleep, leading to the individual being tired during the day, reducing their sexual interests and capabilities.
Memory Loss and Troubled Focus
Several studies have shown that sleep apnea is associated with cognitive dysfunction, which is characterized by the impairment of memory, and poor focus and attention. This is no surprise since adequate sleep improves memory and cognitive power.
Sleep Apnea and Brain Performance
Our body has what is known as a “lymphatic system” to drain out our body’s waste and toxins at all times, but the brain’s waste disposal system only works efficiently during sleep. During sleep, the brain cells actually shrink to allow the cerebrospinal fluid to flow 10 times faster in between brain cells than when we are awake, leading to improved executive skills including:
- Concentration
- Attention and reactivity
- Decision making
- Problem solving
- Learning and memory
- Creativity
- Coordination
- Social skills
- Overall mood and health
Sleep apnea leads to interrupted sleep, therefore hindering proper brain rejuvenation. Also, the brain cleaning works to remove neurotoxins, specifically harmful ones such as the one called Beta-Amyloid, a dangerous waste that is formed as a result of using the brain all day, every day. This is not an excuse to shut off your brain during school or work, but it is a reason for you to get to bed on time.
When Beta Amyloid is not cleaned out, it accumulates and, overtime, forms plaques. Scientists at the Stanford University School of Medicine found that beta amyloid plaques cause Alzheimer’s disease. This is why individuals with sleep apnea have an increased risk for Alzheimer’s disease.
Hypersomnia (Daytime Tiredness)

Obstructive Sleep Apnea ranges from a few to as many as 100 stops in breathing and awakenings.
Upon airway collapse and bringing a stop to your breathing, the brain senses a drop in blood oxygen and compensates by waking your up, therefore disrupting rest and rejuvenation. Inevitably, this leads to you feeling a major lapse in energy during the day, and increases your daytime sleepiness as the body is sleep deprived and wants nothing more than to hibernate in a cozy bed.
Signs of daytime sleepiness include suddenly dozing off, excessive yawning, and difficulty keeping your eyes open. Excessive daytime sleepiness is associated with impaired work performance, fatigue, poor concentration, and an increased risk of drowsy driving. None of these sound appealing, do they?
Often people mistake daytime sleepiness for normal day-to-day tiredness, low energy and poor focus. However, ignoring such symptoms lead to undiagnosed sleep apnea and an increased risk for potential health and wellness complications.
Mood Changes
Mood changes in sleep apnea are related to lack of emotional and mental rejuvenation due to poor sleep. Sleep deprivation depletes the happy neurotransmitter, serotonin, while increasing stress hormones, likely leading to irritation and an overall negative mood. Sleep apnea has also been linked to various levels of depression.
Choking and Gasping for Air During Sleep
A 2013 study found that nighttime gasping, or choking, is the most reliable indicator of obstructive sleep apnea, whereas snoring is not very specific. Another study found a significant, positive correlation between the severity of Obstructive Sleep Apnea and snoring intensity.
Loud Snoring, Dry Mouth, and Sore Throat
According to this study, patients have also reported mouth dryness associated with night time snoring. Snoring is the result of air blowing through a small or partially blocked airway, as in the case of sleep apnea. Loud snoring can be an indication of a more serious airway blockages, compared to a soft snoring which is rarely a cause for concern.
Just Snoring or Sleep Apnea?
Snoring is associated with 80% to 90% sensitivity and 50% specificity, meaning that snoring is not very specific in determining Obstructive Sleep Apnea. Other potential causes of snoring include nasal congestion, enlarged mouth glands (adenotonsillar hypertrophy), abnormalities of the facial bones (craniofacial abnormalities), and obesity.
Overall, sleep apnea is diagnosed based on several symptoms and risk factors, in addition to just snoring. This is why your doctor or a sleep specialist will consider all involved symptoms, health history and risk factors before diagnosing you for sleep apnea.
Morning Headaches

10% to 30% of patients with untreated Obstructive Sleep Apnea report morning headaches. According to this 2015 study, the headache is usually not associated with other common causes of headaches, such as extreme sensitivity to light, nausea or hypersensitivity to sound.
Some studies associated the headache with low oxygenation to the brain during sleep, however, this study found no significant difference in oxygenation in those with sleep apnea compared to those without. Other explanations why sleep apnea causes headaches include reduced blood flow, intracranial pressure, and impaired sleep quality along with too much buildup of carbon dioxide during sleep apnea-related oxygen reduction.
Sleep Disruption and Difficulty Staying Asleep
A normal, goodnight’s sleep involves cycles of 90minutes with five sleep stages in each cycle. Sleep Apnea patients can wake up to 100 times per night. The body responds to difficulty breathing by waking up. These awakening can keep a person in one stage of sleep or unable to get into restorative sleep stages.
According to a recent study, one third of patients with sleep apnea report sleep disruption involving inability to stay asleep. Interestingly, this is more common in female patients. Stops in breathing triggers the body to wake up and, often, it can be harder to fall back asleep, leading to a pretty inadequate sleep overall.
Nighttime Urination (Nocturia)
In a 2016 study, it was reported that patients with sleep apnea had a high frequency of urination during the night. When patients started sleep apnea treatment, the frequency of urination reduced in 85% of the participants. While all participants had no other voiding causes, more research is needed to confirm a causal relationship between sleep apnea and nighttime urination.
Symptoms Due to Related Complications
Some patients may report symptoms associated with complications of sleep apnea such as symptoms of heart problems, diabetes, cognitive decline, and depression. For example, people with long-term undiagnosed sleep apnea may experience chest pain, induced by sleep apnea. Qualified health care professionals are always on high alert when it comes to sleep apnea symptoms and there’s still plenty of questions still to be answered.
Effects of Sleep Apnea
Not getting the sleep your body needs can have some less than appealing side effects. Proper sleep is essential, and sleep apnea can lead to some pretty dangerous situations, such as drowsy driving, increased depression, Type 2 Diabetes, myocardial infarction (more commonly referred to as a heart attack), congestive heart failure, and strokes. All these instances can result from your sleep deprivation and your body’s desperate attempt to make up the difference. But what are the short-term and long-term effects of sleep apnea?
Short-Term Effects of Sleep Apnea
Drowsy Driving

On a short-term level, sleep apnea will lead to drowsy driving, poor cognitive performance and extreme exhaustion leading to reduced productivity and accidents.
A 2007 study found that motor vehicle accidents are two to three times more common among patients with Obstructive Sleep Apnea than those without it. According to a systematic review in the Journal of Clinical Sleep Medicine, sleep apnea significantly increases the risk of road accidents, which makes sense since those with sleep apnea are not only drowsy, but also have a much harder time focusing on, well, anything.
Due to the impact of sleep apnea on the brain, leading to poor cognitive function, drowsy driving, and accidents, it’s important to always be paying attention to your symptoms. While this probably goes without saying, do not drive when you feel drowsy. You won’t be doing yourself or those on the road any favors.
Long-Term Effects of Sleep Apnea
Depression
A 2012 study carried out a National Health and Nutrition Examination Survey. The survey asked 9,714 adults questions regarding frequency of snoring, snorting, gasping, or stops in breathing while asleep and completed further screening questions about depression symptoms. The study found that frequent snorting/stops in breathing was associated with probable, major depression.
A 2013 follow up study confirmed the link between sleep apnea and depression. The study recommended regular psychiatric screening among patients with Obstructive Sleep Apnea to prompt the timely detection of depression.
Heart Problems and Stroke
A 2017 study revealed a causal association between obstructive sleep apnea and heart problems. There is a consensus in research evidence to show that patients with moderate to severe, untreated, Obstructive Sleep Apnea, are at an increased risk for various heart-related problems including high blood pressure, coronary artery disease, cardiac arrhythmias, heart failure and stroke.
According to a recent study, the prevalence of pulmonary hypertension (or right-sided heart failure) among patients with obstructive sleep apnea ranges from 17% to 53%.
Type 2 diabetes

Obesity is a risk factor for developing diabetes, and several studies have confirmed that obstructive sleep apnea alone can increase the risk for diabetes, regardless of the existence of obesity. In this study, about 12% of patients with obstructive sleep apnea developed diabetes over a 67-month period.
Patients with severe obstructive sleep apnea had an approximately 30% higher risk of incident diabetes compared with patients without Obstructive Sleep Apnea.
Metabolic Syndrome
Metabolic syndrome manifests as high blood pressure, high cholesterol levels, high blood sugar, and excessive weight. Studies suggest that sleep apnea may be a manifestation of metabolic syndrome.
Nonalcoholic Fatty Liver Disease
According to a study conducted in Turkey, patients with severe sleep apnea have a two to three times greater risk for developing Nonalcoholic Fatty Liver Disease.
Sleep-Deprived Partners
Loud snoring, choking, or gasping for air during sleep will disrupt nighttime rituals for even co-sleepers. Wearing earplugs and using a whitenoise machine are effective coping strategies, but, most importantly, partners should encourage the person they are sleeping with to get checked, or tested, as the snoring and choking will get better with treatment, and much worse without it.
Worsening of ADHD
Attention Deficit Hyperactivity Disorder (ADHD) is a chronic condition that causes inattentiveness, mood swings, tiredness, restlessness, trouble focusing and sitting still, and controlling impulses. These symptoms are similar to how individuals with sleep apnea may behave during the day, according to this 2019 study. Therefore, sleep apnea may go undiagnosed, leading to sleep disruption. This is particularly bad since sleep disruption worsens ADHD symptoms.
Treatments for Sleep Apnea

Treatments for sleep apnea may involve resolving the underlying cause of sleep apnea, such as suggesting an air delivery machine to prevent breathing stops, oral devices and positional change to improve air flow. Lifestyle changes and surgery might be recommended for more complicated cases.
But the bottom line is that sleep apnea is a treatable condition. According to clinical guidelines, sleep apnea treatment combines lifestyle modification with individual specific medical therapy. Continuous Positive Airway Pressure (CPAP) machines are often a part of initial treatment for severe cases of Obstructive Sleep Apnea.
Alternatively, patients with mild sleep apnea who prefer not to use, or do not respond well to, airway pressure machines can choose to try oral appliances as a treatment alternative.
If all of this sounds like gibberish to you, fear not. We go into much more in-depth explanations of these sleep apnea treatments below.
Obstructive Sleep Apnea Treatments
CPAP Machine
CPAP stands for Continuous Positive Air Pressure. According to a recent study, CPAP is the current leading, and most effective, therapy for Obstructive Sleep Apnea.
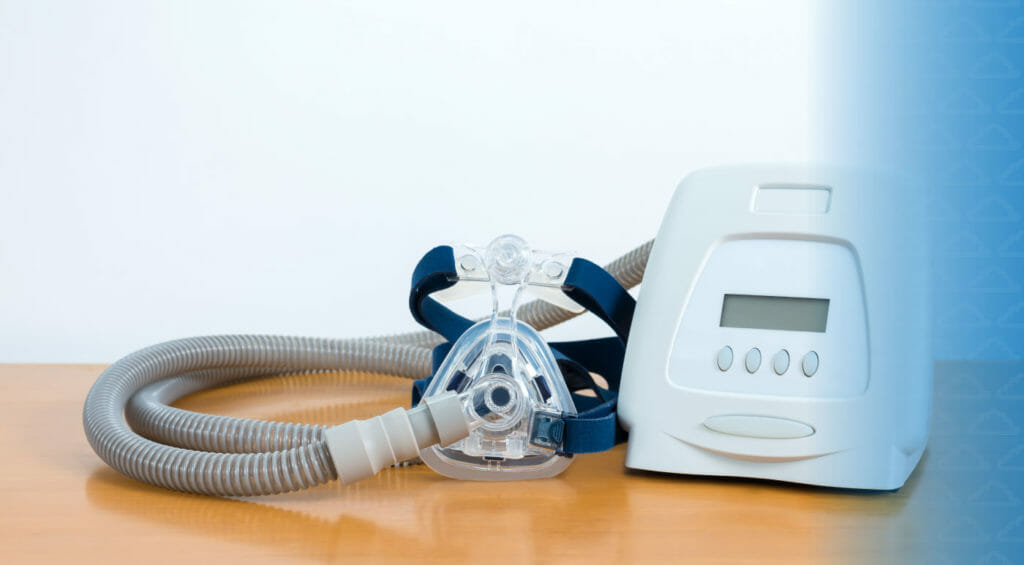
A CPAP machine is a specialized box that has a regulated fan to draw air from the room to allow a certain amount of air pressure to blow through the person’s airways, while also filtering out any impurities in the air such as dust or smoke. A doctor or sleep specialist will give you a prescription for a specific air pressure setting as well as for a specialized machine and mask used to deliver the pressurized air flow.
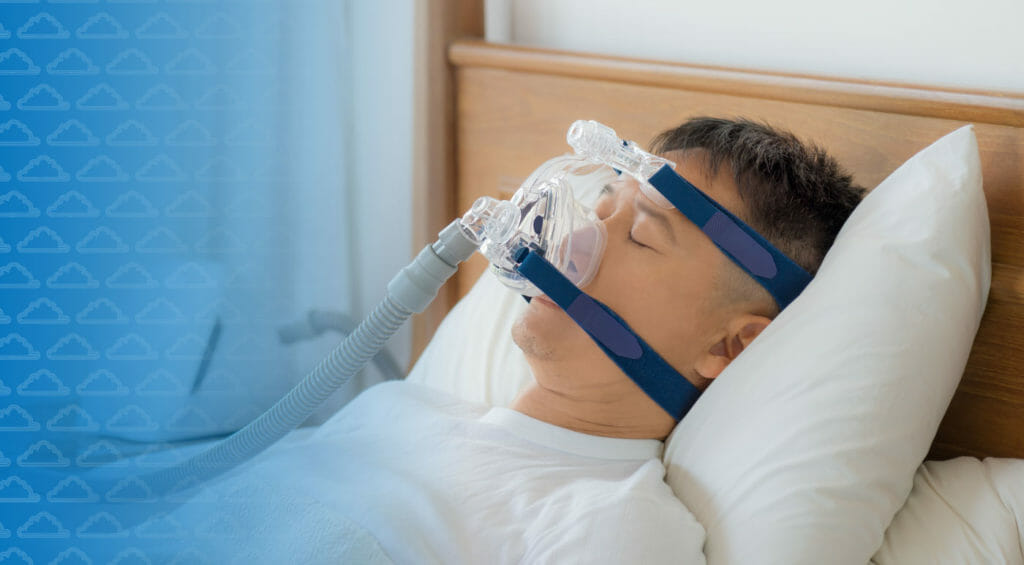
Based on prescribed settings, the right amount of air is gently pushed through the CPAP machine humidifier and then through the specialized CPAP tube and mask attached to the machine. This gentle push of air solves the issue of the collapsed airway, which is the main characteristic of Obstructive Sleep Apnea.
According to a 2014 study, the CPAP works by continuously, and gently, pushing pressurized air though the airway to prevent the individual’s airway from collapsing to improve sleep quality and overall positive health outcomes.
CPAP Side Effects
Research shows that CPAP machines have been used for over 30 years with success. Most side effects are minor and can be alleviated with easy strategies.
Common side effects include eye irritation, conjunctivitis, skin ulceration, skin discoloration (lightening or darkening) and discomfort or irritation at the site where the mask contacts the skin. Here are tips to address common CPAP side effects:
- Adjusting the Fit: Proper fitting and refitting with change in weight or as the person/child grows will prevent air leaks and minimize pressure on the face and avoid facial and eye irritation.
- Humidify the Air: Many CPAP machines come with a built-in humidification chamber where the water is warmed before it travels and pushes through airways. Humidified air soothes and moistens nasal and throat passages, to prevent dryness and nasal congestion. This is important, especially when the air is dry.
The humidifier chamber is easy to maintain and clean. You can also use nasal saline spray to help reduce congestion and irritation in nasal passages.
- Customize Mask, Tubing, and Straps: Having a well-fitted mask is important, as is having the right tubing and straps. The most common mask covers the mouth and nose but you can also get the masks that have separate nasal and oral aspects. This way you can switch masks based on your needs.
CPAP tubing tends to be long, allowing you a little room for movement. You can make your CPAP tubing heated to keep the air temperature warm as it travelled from the room into your airway. This will prevent the air from getting cold during the travel and work hand-in-hand with humidification efforts to create moist and soothing air reducing congestion, irritation and drying of the mouth and nasal passages.
- Keep it All Clean: It is important to keep the CPAP machine, tubing, and mask clear to avoid any air impurities and prevent them from coming through. If you can’t find motivation to clean your CPAP, remember that you are breathing whatever is in the tubes of your machine. You want only clean, warm and soothing air in the tubes, do yourself a favor and clean your machine.
Daily cleaning is recommended and while it may sound excessive, it will help you prevent additional problems including mold exposure, dust build up, bacteria growth and risk for sinus infections or pneumonia, not to mention premature equipment breakdown (which can be expensive to replace).
How To Clean a CPAP Machine: Parts You Must Clean

When cleaning, you must ensure to clean all parts of the CPAP system including mask, headgear, tubing, humidifier water chamber, and the CPAP machine itself. Cleaning is simple, you can easily follow the manufacturer’s instructions. But, for your ease, we listed some general guidelines below…
CPAP Machine Cleaning Components:
You will need: clean warm water, a soft and clean cloth, dish soap (preferably mild antibacterial), a small sink or tub, and a dry towel (make sure it’s also clean).
First, unplug the machine, disconnect the headgear and mask from the tubing, remove the humidifier chamber if it is removable, and empty out any leftover water from the humidifier.
Secondly, use a clean towel to wipe down any build up of dust around the machine.
Thirdly, fill your clean sink, or tub, or basin with clean, warm water containing mild soap. Using a clean towel, clean (or soak for 20-30minutes) the mask and headgear. Clean CPAP tubing using warm water and by passing the warm water through the tube a couple of times to flush through any built-up bacteria. Also, cleanse the humidifier chamber with warm water. Allow everything to air dry.
Ways to Manage CPAP Machine Sound
CPAP machine make significant noise due to air movements and the sound of the machine itself. But fear not, there are things you can do to reduce the noise…
- Machine Position: Keep your CPAP machine away from you and below ear level. This will immediately reduce the amount of sound your ears receive. You can also have a clean, folded towel underneath the machine to muffle some noise. Make sure the towel doesn’t block the air entry. Air entry is what allows the air in, and anything near the air entry will affect the air quality and the amount of air your recieve.
- Reduce Air Leaks: CPAP machines have a multitude of connections, from the machine, to the tubing, to the mask. Air leaks increases the overall system noise. Ensure that everything is well connected, but also that the mask is still not too tight.
- Check the CPAP Humidifier: If the water in the humidifier is running too low, you might hear a lot more noise than when the water is full.
- Use White Noise: White nose is a sound that masks other sounds, such as the whirr of a fan or specialized white noise machines. Since sleep is simply a change in your brain waves, sounds act directly on those brain waves. While there are certain sounds to help you sleep, others can actually keep you awake or negatively affect your sleep.
White nose can help balance out disorganized noise from the CPAP machine. While comparing the incidence of white noise on sleep among ICU patients, this study found that patients had fewer awakenings with white noise compared to irregular hospital sounds.
Other Airway Pressure Devices (BPAP)
Bi-level positive airway pressure devices are also effective treatments for Obstructive Sleep Apnea. BPAP provides higher air pressure on inhale and less pressure on exhale.
Alternative Treatments to CPAP Machines
Oral Devices
While CPAP is the most effective treatment for sleep apnea, oral devices are an option for mild sleep apnea when an individual is not interested in pursuing CPAP.
Mandibular Repositioning Devices
Mandibular reposition devices aim to increase breathing space in the mouth and throat. Many studies have compared these types of devices to lifestyle changes and other conventional treatments such as CPAP. This study found no significant improvement in sleep apnea outcomes from mandibular repositioning devices, but it would be worth talking to your doctor about whether one might work for you.
Surgery
A recent study insists surgery is only a good option if other treatments have failed. Surgery aims to correct anatomical problems in the face, nose, throat muscles, and other parts of the airway to increase airflow. Complications of surgery vary based on the person’s risk and the part of the body being operated on.
Behavior Modification and Lifestyle Changes
Stop Drinking Alcohol

According to this study alcohol consumption increases the frequency and duration of obstructive sleep apnea episodes. In addition, alcohol negatively affects your REM sleep, even in people with a low risk of sleep apnea. When people stop drinking alcohol, they often see a marked decrease in the severity of sleep apnea.
Sleep Position
Sleeping on your side prevents your tongue and throat tissues from collapsing and partially blocking your airway. This position further ensures that your mouth is wide open for effective breathing throughout the night. In this study, patients reported worsened sleep apnea symptoms in a spine position and improved symptoms with side positioning.
Quit Smoking

According to this 2019 study, long-term smoking cessation leads to improved sleep quality and a lower risk of sleep-disordered breathing.
Positional Therapy
According to a recent study, avoiding sleeping on the back (also called positional therapy) is effective in coping with Obstructive Sleep Apnea caused by position changes. Your sleep specialist or doctor will determine if your sleep apnea (should you be diagnosed) is caused by position change and if position changes–like the ones listed below–can help.
Lose Weight

According to this 2019 study, weight loss often helps to improve your blood pressure, your joints, and your overall health, which helps mitigate all the risk factors associated with sleep apnea.
Weight loss is a process. Start with a regular exercise routine, like going for a short morning walk or parking a few extra blocks away from your office. Talk to your doctor about other options you’d also like to consider.
Liaise With Prescriber to Assess Medications Effects
If you notice worsening of sleep apnea symptoms after starting certain medications, connect with a prescriber and reassess. Certain medications have been shown to worsen the severity of sleep apnea. These include medications belonging to benzodiazepine receptor agonists, barbiturates, other antiepileptic drugs, sedating antidepressants, antihistamines, and opiates.
Tennis Ball Trick

Sleeping on your back makes sleep apnea worse. The tennis ball trick helps avoid sleeping on your back. In this study, patients reported worsened sleep apnea symptoms in a spine position and improved symptoms with side position.
How does it work? A tennis ball is worn by either being sewn into a shirt or attached to the bed to prevent the individual from sleeping on (or rolling onto) their back. According to a study published in the journal of sleep medicine, the “tennis ball trick” improved breathing outcomes. However, another study found that the use of a tennis ball declined after the initial start.
Playing the Didgeridoo

A 2006 randomized control study found people who trained their upper airways by playing didgeridoo instruments for four months reduced daytime sleepiness in people with snoring and obstructive sleep apnea syndrome. Researchers concluded that didgeridoo playing opened up the upper airway, allowing better breathing at night. Furthermore, partners of participants in the didgeridoo group were much less disturbed in their sleep.
While none of these is a sure fix (even the didgeridoo), they can all contribute to improvement if done with proper medical supervision.
Sleep Apnea in Children
In children, Obstructive Sleep Apnea is recognized by the same symptoms and risk factors as in adults. Narrowing of the airway and obesity are the main risk factors, with a few differences…
Causes of Sleep Apnea in Children
The most common causes of sleep apnea in children are congenital myasthenic syndromes and muscular dystrophy, which causes significant muscle weakness leading to difficulty breathing at night.
Treatments for Sleep Apnea in Children
Continuous Airway Pressure (CPAP)
Current clinical guidelines recommend CPAP for children with minimal airway obstruction or who continue to experience severe obstruction even after surgical correction.
Similar to adults, a sleep specialist would be involved in choosing the right machine, the right mask, and the right pressure.
Adenotonsillectomy (Surgery)
Adenotonsillectomy refers to surgical resection of the tonsils and adenoids to widen the airway for better airflow to prevent obstruction during sleep. A 2013 study showed that adenotonsillectomy leads to reduced symptoms compared to waiting to see if the situation improves as the child grows up (also called “watchful waiting”).
Current clinical guidelines recommend identifying and pursuing the right treatment as soon as possible. Waiting could mean the worst case scenario for the child. Like in adults, surgery is a last resort and recommended when other treatment options have failed or not been applicable.
Orthodontics — Rapid Maxillary Expansion (RME)
In children with narrow airways, orthodontic treatments widen the palate and nasal passages, leading to increased airway flow and reduced obstruction during sleep. This study found that orthodontics, especially when done prior to the maturation of the jaw (around puberty) can be effective in reducing abnormal breathing during sleep.
Medications (Intranasal Corticosteroids )
According to a 2001 randomized control trial, in children with mild to moderate obstructive sleep apnea, several studies have shown beneficial effects of intranasal steroids and montelukast, as an addition to surgically widening the airway.
Environmental controls
Air impurities from smoke, indoor allergens and other indoor pollutants cause nasal congestion and increase airway resistance. These factors should already be avoided, but especially when it comes to children. To improve quality of sleep, focus on practicing good sleep hygiene and other environmental controls, including having an optimal mattress made for children.
When To See Your Doctor
If you currently experiencing symptoms outlined in this article, it is time to see your doctor, or sleep clinicians, for further investigation and treatment options.
Preparing for Your Doctor Appointment
So, at this point, you’ve likely come to the conclusion that either you don’t have sleep apnea, or you do. For those of you that have decided it’s time to make a doctors appointment to get tested, here are some things you should prepare for…
Know Your Symptoms and Information
The doctor or a sleep specialist will ask you various questions around your snoring, sleep patterns, and day time function. Your doctor will also ask about your medical history and diagnosis. Likely, they will ask you if you have diagnosed hypertension. They will also ask about your weight and risk factors such as smoking, alcohol and also about health history.
Make a list of all symptoms if you can prior to appointment. Specific answers help in accurately diagnosing Sleep Apnea and understand the severity, which helps get to the best treatment option.
Know Your Medication and Supplements
Make sure you know all the medications, vitamins, or supplements you are currently taking. This will provide your doctor insights into other conditions you may have or if medications or supplements would interfere with the proposed treatment based on your situation.
What to Expect from Your Doctor or Specialist
Expect the practitioner to be very specific and be ready to answer follow up questions. Symptoms of Obstructive Sleep Apnea may be similar to other health issues, so the goal is to make a proper diagnosis while ruling out any associated health issues. For example, Gastroesophageal Reflux Disease (GERD) can mimic OSAS by producing a choking sensation and trouble breathing at night.
It can help to ask a partner or co-sleeper for insights. In addition, you can keep a sleep journal to record how you feel upon waking up and any awakenings you remember.
The doctor might refer you to a sleep clinic or sleep specialist for a more thorough assessment, based on the clinical presentation.
Questions to Ask Your Doctor

You can ask your doctor about your risk factors for other conditions that share symptoms with Obstructive Sleep Apnea, such as endocrine disorders. The doctor will determine a diagnosis based on your health history, age, and risk factors. You can also ask the doctor if they recommend further testing, and ask for resources available to help people in your situation.
Testing for Sleep Apnea
If you’re not sure whether or not you’re actually dealing with sleep apnea (versus just the everyday monday blues), there’s doctor-regulated sleep studies you can participate in to confirm your sleep apnea diagnosis. Other tests to confirm whether or not a person is suffering from sleep apnea includes EEG (Electroencephalogram), EMG (Electromyogram), EOG (Electro-oculogram), ECG (Electrocardiogram), nasal airflow sensors and even snore microphones.
Testing and Diagnosis
According to a 2014 study, a sleep study is the standard for diagnosis and exclusion of sleep apnea. This study is also called polysomnography (PSG).
What Is a Nocturnal Polysomnography?
A sleep study, also called polysomnography (PSG), is a test done to diagnose Obstructive Sleep Apnea.
Sleep studies are also used in combination with other clinical assessments and tests to diagnose a variety of other sleep disorders, including narcolepsy, sleep-related movement disorders, and certain parasomnias.
According to current clinical guidelines, a sleep study is recommended for people who experience regular daytime sleepiness and the presence of at least two of the following clinical features of Obstructive Sleep Apnea: habitual loud snoring, gasping or choking during sleep, and diagnosed systemic hypertension.
How Does a Sleep Study Work?

During a sleep study, the patient sleeps with electrodes attached to their head and body. The electrodes monitor a variety of physiological variables, including brain waves, sleep stages, respiratory effort, airflow, presence and absence of snoring, oxyhemoglobin saturation, electrocardiography, body position, and eye and limb movements.
Doctors use all of this information to understand what’s affecting your sleep and how to fix it.
The sleeping room has a complex video and audio system that allows the technologist to see, hear, and communicate with the patient without entering the bedroom.
Split-Night Study
Split-night studies are similar to full-night testing, except the diagnostic portion of the study is performed during the first part of the night only. This is preferred by many, but the examiner might recommend a full night study if longer observation is required.
How to Prepare for a Sleep Study
If you’re going to take part in a sleep study, the sleep specialist will give you instructions. It’s very important not to have any caffeine before your sleep study.
Consuming caffeine, whether it’s in the form of food or drinks, such as coffee, can affect the results of the test and hide an underlying sleep disorder. Based on findings from this study, you should abstain from caffeine for six to eight hours before the sleep study.
If you’re feeling anxious about a sleep study, it can help to have a tour of the sleeping room ahead of time. You can even watch a video online to get an idea of what it will be like, and you can talk through any anxiety with your doctor or nurse.
You can also bring your own pillow to the sleep study to make yourself more comfortable.
How Much Does a Sleep Study Cost?

The cost of a sleep study depends on whether it happens in your own home or in a laboratory. A laboratory-based sleep study costs more than a home-based study.
The cost of laboratory-based sleep studies ranges widely, from $500 to $3,000, based on your insurance coverage in your country or state.
Home-based sleep studies are not as in-depth but provide enough information for your doctor to make treatment decisions. You will be given a portable machine and instructions on how to record your own sleep. You will be charged for the equipment rental, physician assessment fee, and disposable devices used during the test, so the fee can range significantly.
Other Tests for Sleep Apnea
Sleep specialists may use EEG to record and evaluate brain wave activity, to assess the severity of Obstructive Sleep Apnea on their patient’s brain.
EMG (Electromyogram)
Sleep specialists use EMG to confirm the presence of REM sleep. EMG captures REM sleep-associated movements such as twitches, teeth grinding, and leg movements.
REM sleep is an important sleep stage where brain rejuvenation, and dreaming occur. REM sleep triggers active brain and body activities, including eye and other body movements. In REM, the muscles are paralyzed to protect the sleeper from movement-related accidents.
EOG (Electro-oculogram)
EOG is used to record eye movements associated with REM sleep.
ECG (Electrocardiogram)
Diagnosed systemic hypertension is one of the diagnosing criteria for Obstructive Sleep Apnea. In addition, sleep deprivation caused by Obstructive Sleep Apnea leads to poor heart health. ECG is thus used to record heart rate and rhythm.
Nasal Airflow Sensor and Snore Microphone
Nasal airflow sensors records airflow while snore microphones records, naturally, snoring activities.
Living With Sleep Apnea

Living with sleep apnea can look impossible at first. However, with many treatment options to choose from, life can be even brighter and happier as you get a better night’s sleep and, as a result, much more productive days. Get to know your CPAP machine and apply strategies discussed in this article to reduce difficulties when using CPAP. Keeping in touch with your doctor and repeating sleep studies as needed to monitor your progress is also key.
Final Thoughts
A growing body of research shows that Obstructive Sleep Apnea is an increasing and dangerous sleep disorder that significantly increases an individual’s blood pressure, hypertension, chances of stroke, depression, and mortality.
Lucky Obstructive Sleep Apnea is treatable. However, untreated sleep apnea can lead to serious health conditions and even death. The best bet is to address any symptoms with your doctor as soon as possible and undergo treatment as needed. Also, if you are at risk but do not have symptoms, prioritize lifestyle modification to maximize prevention.